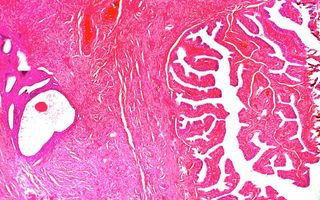
Endometriosis, a condition in which uterine tissue grows outside the uterus, is commonly treated with hormone therapy. However, a team of researchers at Yale has found that hormone therapy may not be the best first-line treatment for all women diagnosed with the condition, opening the door to the possibility that more effective and targeted treatments may be available to some women.
Endometriosis affects 10% of reproductive-aged women, and it causes significant chronic pain that in some instances is so debilitating, that surgery may be required to remove the additional uterine (also called endometriosal) tissue. Standard first-line treatment for endometriosis can include painkillers, but almost always includes hormone therapy, specifically progestin therapy. Hormone treatment is believed to slow the growth of endometriosal tissue, and prevent new tissue from implanting.
In a new study published in the Journal of Clinical Endocrinology & Metabolism, researchers showed that the effectiveness of the progestin therapy depends on whether a woman’s endometriotic lesions have the progesterone receptor (PR). The researchers tested the endometriotic lesions of 52 women who had undergone surgical evaluation for endometriosis, and they found a significant association between PR status and responsiveness to progestin-therapy. Those whose endometriotic lesions were PR-positive responded much better to the progestin-therapy, while those whose lesions were PR-negative found little relief from progestin-therapy alone.
From these findings, the research team concluded that knowing a woman’s PR-status may help them develop a “novel, targeted, precision-based” approach to treating and managing endometriosis individually. “Receptor status in endometriosis could be used in a manner analogous to the use of estrogen/progesterone receptor status in breast cancer for tailoring hormonal-based regimens,” said Dr. Valerie Flores, first author and clinical instructor at the Yale School of Medicine.
This is particularly important for the treatment of a painful disease, because it means women who are suffering chronic pain may not need to go through the first step of trying progestin treatment to test whether they respond. They may immediately get tested for the presence of the progesterone receptor, and pursue targeted treatment based on their individual needs. This is particularly important for a disease that can wreak havoc on women’s daily quality of life.