What Gut Bacteria Does with the Food and Drugs We Give It
With alarming implications for human health.
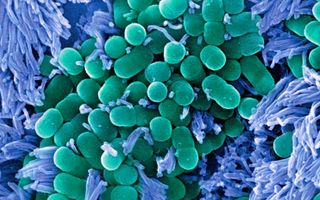
You’ve probably heard about the human microbiome. It’s the collection of microscopic bacteria that lives all over and inside of the human body, particularly in the stomach and intestines, and works to help keep us alive. We’ve known about it for a long time, and scientists have increasingly suspected it plays a large role in keeping us on an even keel, but we haven’t known much about how.
Enter, a team of researchers at the European Molecular Biology Laboratory in Germany. Led by Peer Bork, Kiran Patil and Nassos Typas, the team has mapped the diets and activity of most gut bacteria species and, more startlingly, discovered non-antibiotic drugs may be contributing to antibiotic resistance.
To do so, they developed a laboratory model of a healthy, human gut consisting of 96 strains of 72 of the bacterial species most common to the gut. They then cultured each strain in various substances to discover what the microbes do with what we put into our bodies.
“Now we know what the bacteria need, or what they do not like,” Patil said. “What they can utilize, what they can throw out of the cells, and what they can break down into nutrients inside the cell and [what they use those nutrients for]. You can compare this to a road map of a city: where you can enter, and where you can leave, and where you can go inside.”
It’s a map that also helps scientists understand what bacteria might be taking from everything we put into our bodies — including medicine. In addition to determining what, and how much of it, each bacteria strain needs to thrive, the researchers exposed the bacteria to 1,200 different, common medications. Non-antibiotic drugs (as opposed to antibiotics, which target invasive, ‘bad’ bacteria) are designed to interact with human proteins, not bacteria. But if the drugs, via ingestion, interact with gut bacteria first, whether they work as intended is in question; it could be that the products of gut bacteria metabolizing the medication is what actually has an effect.
“For many of the drugs, it’s likely the mode of action might be via the microbiome,” Patil explained.
In testing these medications — which included common, over-the-counter drugs, antidepressants, antipsychotics, antibiotics and more — the researchers noticed something strange: 25% of non-antibiotic medications produced the same side effects as antibiotics (for example, diarrhea), as they damaged at least one species of good gut bacteria.
“Of course we found that antibiotics also kill the growth of gut bacteria, that is well-known, that is expected,” Patil said. “But what we found is that almost one-quarter of the [non-antibiotic] drugs are also affecting the growth of gut bacteria.”
His colleague, Bork, called it “collateral damage.”
The team also found bacteria resisted antibiotic and non-antibiotic drugs in the same way, suggesting even non-antibiotic drugs may be contributing to the spread of antibiotic-resistant strains.
“We don’t want to raise false alarms. Many of these drugs are in active use, and people take drugs all the time for different purposes,” Patil said. “Of course we want to say this needs to be investigated, but this should not be taken as medical advice. It’s not like people should stop taking their medications because of the fear of antibiotic resistance.”
At this point, the findings should inform further research into antibiotic resistance and be taken into consideration by public health policymakers. It can also provide a foundation upon which to study how to use existing drugs more effectively, or to develop new medications, to tweak the microbiome in order to get desired, healthy results. Patil points to earlier research that mistakenly concluded Type 2 diabetes changes a person’s composition of gut bacteria; later research revealed it was the diabetes drug metformin that affects the gut micro biome, not the metabolic disorder. His research, he says, finally starts explaining this.
But only starts.
“This is just the beginning,” he said.
Liesl Goecker is The Swaddle's managing editor.
Related

Essential Medicines Are Missing from Maharashtra’s Pharmacies
