Electric Shock Treatment Is Still Controversial, But Not For the Reasons People Think
“The procedure has been so horrifically portrayed in media…showing it being used in mental facilities as punishment, not for its tremendous therapeutic effects,” one researcher said.
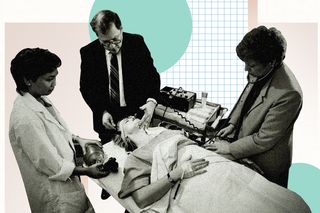
Electroconvulsive therapy — a medical treatment using electric shocks to treat mental health issues — is a controversial, last-ditch treatment effort in cases where other forms of medication have not worked. In the early 1900s, when ECT was first used, patient-focused issues such as consent were often overlooked, which associated connotations of torture to ECT. Evidence shows ECT was also used to control unruly patients in mental asylums to maintain order, historian Jonathan Sadowsky, writes for Scientific American. This led to a cultural distrust of ECT as a valid mental health treatment, drawing up the image of screaming, bucking people being administered electric shocks by force.
Today, however, ECT has come a long way from its torturous roots, both in terms of how the procedure is administered, and how it is understood. ECT became a widely-accepted, modernized procedure since the 1980s, when it started being administered with patients’ consent on a large scale, with the help of anesthesia that prevented them from feeling pain, and muscle relaxants that kept their muscles from reacting violently to the electric shocks, thereby preventing fractures and injuries. With the inception of ECT’s more humane avatar, public perception of the procedure also changed, with the medical community and a more trusting patient base endorsing the procedure.
Today, ECT is most commonly used to treat severe major depression, bipolar disorder, and schizophrenia. The treatment involves passing currents through a patient’s brain to trigger seizures. The procedure is believed to change patients’ brain chemistry in ways that have shown to produce a partial or complete reversal of poor mental health states.
The main controversy surrounding modernized ECT is a lack of conclusive scientific research that establishes the safest parameters for administering ECT. “The neuroscience is completely unknown. It’s baffling to me,” Wendy Marie Ingram, a U.S.-based psychiatric epidemiologist, tells Scientific American. Who should be administered ECT, how much electric current should be given to patients, which side of the brain responds best to the shock treatment, how often patients should receive it, what are the side effects of the procedure, and how widely, and well, are the anesthesia and consent rules being followed by ECT providers — are all questions that have not been conclusively answered by research yet, thereby shrouding the procedure in suspicion.
As a result of this uncertainty, some life-long critics of ECT are advocating for its complete suspension — a recent study, published in Ethical Human Psychology and Psychiatry, that meta-analyzed the existing evidence for the efficacy of ECT for depression found it severely lacking. Its lead author, Dr. John Read from the University of East London, told the BBC that the evidence recommending ECT for depression is “the lowest quality of any I have seen in my 40-year career.”
Related on The Swaddle:
It’s Time For a More Humane Approach to Mental Health Care
This, however, is at odds with how medical professionals around the world describe their patients’ near-instantaneous recoveries with ECT. “The procedure has been so horrifically portrayed in media…showing it being used in mental facilities as punishment, not for its tremendous therapeutic effects,” Ingram says. Whilst acknowledging the gap in medical understanding of the safest ways to administer ECT, Ingram says she has herself witnessed “patients who are severely depressed, suicidal or catatonic are given ECT and two weeks later they are up, happy, chatting with the physicians and nurses.” Patients — most studies say 58–70% of all who receive ECT — report feeling fewer symptoms or none at all after the treatment.
This discrepancy can be explained by uncertainty surrounding how ECT works — while doctors and patients alike can attest to positive ECT outcomes, scientific research has not been able to explain them. Theories, of course, abound — ECT increases the release of hormones that are otherwise disturbed by depression; the procedure helps to rebuild certain brain areas damaged by mental health issues; or that the seizures induced from ECT are likely resetting the brain (most likely temporarily) that offers relief, as concluded by a 2011 review published in the Canadian Journal of Psychiatry, by psychiatrist Tom Bolwig.
And so, in the absence of confirmation of these theories, critics such as Dr. Read explain these positive outcomes as a mere placebo effect. But most of the scientific community, including major medical institutions around the world, choose to focus on the positive outcomes, effectively endorsing the procedure as a valid mental health treatment, for when all else fails.
There is another point of contention in the ECT controversy — that of brain damage, and severe, long-lasting memory loss. According to the American Psychiatric Association, ECT treatment has been associated with short-term memory loss, after which some patients have difficulty recalling weeks (or more) that passed before their treatment. According to the APA, most patients get their memory back after a short while, but some have experienced longer-term, permanent gaps in memory. This is one of the major reasons people still hesitate before opting for ECT, medical historian Sadowsky tells Vox. “The side effects of antidepressants are not pleasant, but most people regard severe memory loss as a much bigger risk. People feel, and I think very rightly, that their memories make them who they are.”
Even Carrie Fisher, who was a strong proponent of ECT, wrote in her memoir Shockaholic, “the truly negative thing about ECT is that it’s incredibly hungry and the only thing it has a taste for is memory.”
Even with the side-effects, however, post-ECT data is largely reported by patients, with no conclusive evidence that the procedure damages the brain permanently, let alone data that can paint a better picture of how frequently patients experience these side-effects.
In the end, what we’re left with is a procedure that seems to work for a majority of patients, which could have some short-term, relatively harmless side-effects, and some potentially harmful long-term ones. Scientists don’t have conclusive data for these phenomena, which has led some to advocate for banning the procedure, and most to continue endorsing it based on real-time patient data.
While we wait for scientific research to catch up to ECT’s complicated legacy, patients are left with a decision to make.
Rajvi Desai is The Swaddle's Culture Editor. After graduating from NYU as a Journalism and Politics major, she covered breaking news and politics in New York City, and dabbled in design and entertainment journalism. Back in the homeland, she's interested in tackling beauty, sports, politics and human rights in her gender-focused writing, while also co-managing The Swaddle Team's podcast, Respectfully Disagree.
Related


U.S. CDC Adds New Symptoms for Covid19 to Its Official List
