
Untrending: If You’re Already Healthy, You Don’t Need Kombucha or Kefir
And even if you’re unhealthy, probiotic drinks might not contain the bacteria you need.

Probiotic drinks and supplements are like the 1950s film The Blob: they’re everywhere, on every menu and increasingly in every fridge. Kombucha, kefir, yakult and more are surrounded by grandiose claims of health benefits.
The only thing is, if you’re already healthy, there’s literally no evidence that probiotic drinks or supplements are going to yield benefits that maintain or improve your health.
In theory, it would seem to make sense. Probiotics are the good bacteria that make up your microbiome, that is, the vast collection of beneficial microbes that live in and on your body that science is increasingly proving are central to human health. Of these, the group housed specifically in the gut is revolutionizing how scientists think about and treat disorders of metabolism (like obesity and diabetes), of digestion (like irritable bowel syndrome), of autoimmunity (like lupus and alopecia), of the mind (like depression and Alzheimer’s disease), and more.
The accepted understanding is that an imbalance in the various strains of bacteria in your gut microbiome, or their improper functioning, is linked to poor health. This has led to a lot of hope, as early evidence suggests altering or reviving a faulty gut microbiome can treat chronic conditions. It has also led to the public belief (aided by advertisement) that probiotics — whether in the pill form or in a drink — are essential to good health.
They’re not; if you are already in good health, you don’t need to worry about maintaining your gut microbiome with the help of probiotic drinks. With a healthy diet, your gut microbiome is self-sustaining. At this point, a probiotic drink becomes redundant. Instead, what’s more important is avoiding, or at least minimizing, things known to damage your gut bacteria: an unhealthy diet, excess alcohol, cigarettes, a sedentary lifestyle, unnecessary antibiotic use, sleep deprivation, and stress.
Related on The Swaddle:
What Gut Bacteria Does with the Food and Drugs We Give It
There is no evidence oral probiotics help you maintain your good health. A 2014 review of 20 clinical trials found that while probiotic supplements containing Bifidobacterium and/or Lactobacillus supplements seemed to shorten the duration of head colds, they had no effect on how frequently participants contracted colds, nor on the severity of their colds.
And while there is some evidence that oral probiotics can help prevent or mitigate post-antibiotic diarrhea, there is about as much evidence that they do not. Plus, one recent study has suggested that oral probiotics may actually prevent the replenishing of gut bacteria for some people following a round of antibiotics.
But beyond this, there’s little to suggest fermented drinks and probiotic pills benefit health. Most contain primarily high quantities of Bifidobacterium or Lactobacillus — two types of good bacteria found in high quantities in most human guts, to be sure. But there’s no guarantee that the included strains of Bifidobacterium or Lactobacillus are the ones that can survive in the acidic confines of the human gut. Even if they are, the health problem you’re trying to solve may be related to one of the estimated 100 trillion other microbes that live in your gut.
“There will probably never be a one-size-fits-all probiotic,” microbiologist Emma Allen-Vercoe, of the University of Guelph in Ontario, told Scientific American in 2017.
Related on The Swaddle:
How the Infant Microbiome Shapes Kids’ Long‑Term Health
That, in fact, is where the real promise of probiotics lies: in individualized and/or disease-specific treatments that target lowering or increasing the amounts of specific strains, or revivifying their sub-par function. But neither these products nor science can fulfill this yet. Scientists are only beginning to map the varieties of human gut flora and their proportions. And what has been discovered so far has limited bearing; for instance, gut microbiota composition varies depending on where a person lives.
Science will also need to determine what type of probiotic gaps and sub-function characterize which disorders. Then we’ll have to figure out how to reconstitute those gaps in effective ways. One of the most encouraging methods is not any kind of probiotic drink or supplement, but rather something known as a fecal transplant. (Yum!) All of this research is underway right now, but it will be a long time before it gets figured out fully.
One thing is for sure, though: None of these probiotic drink and supplement makers have it figured out, either. Which means you should drink kombucha, kefir or yakult only if you like the taste.
Liesl Goecker is The Swaddle's managing editor.
Related

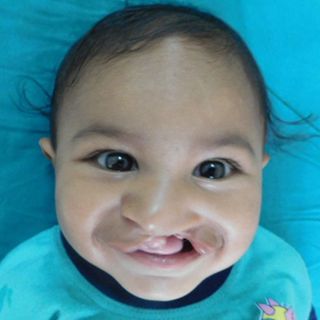
Can You Breastfeed A Baby With A Cleft Lip Or Palate?
