Why the Anti‑Fungal Drug to Treat Mucormycosis Is In Short Supply
The government is regulating the supply of Amphotericin B to prevent its indiscriminate use and black marketing.
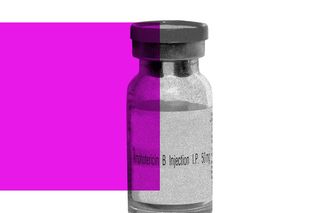
Amphotericin B, the anti-fungal drug used in the treatment of mucormycosis, or “black fungus,” is in short supply across India amid rising cases of infection — prompting hundreds of SOS calls on social media.
Prior to the recent outbreak, there was minimal demand for the drug, leading to it being manufactured only in limited quantities, Money Control reported. But now, depending on their condition, a patient might need four to eight vials a day for 15-30 days — leading to an unprecedented demand for the drug. To meet these demands, a host of pharmaceutical companies have reportedly ramped up productions.
But due to its present shortage, not only have people begun hoarding the drug but also selling it on the black market — at about 5-10 times its original selling price. Meanwhile, several pharmacies have run out of the drug — completely. “Amphotericin B is not available with us. We are getting at least 500 calls daily but can’t do anything if there is no supply. As per a government directive, manufacturers will send the stock straight to hospitals,” Ashok Malik, the proprietor of Malik International Pharmaceutical in New Delhi, told Hindustan Times, adding that his pharmacy ran out of the drug two weeks ago, and hasn’t been able to keep up with the rising demand since.
To prevent hoarding and black market sales, some state governments are trying to procure the drug directly from manufacturers. “The treatment of the infection can be done only in hospitals, so the drug is directly being given to hospitals,” Satyendar Jain, the health minister of Delhi, told the media.
Related on The Swaddle:
A Rare, Serious Fungal Infection Is Complicating Covid19 Cases in 3 Indian Cities
Even without black market sales, the cost of the drug is unaffordable for many. Currently, the drug is available in two forms in India: standard amphotericin B deoxycholate and liposomal amphotericin. And doctors are prescribing the latter because of improved efficacy and fewer kidney and infusion‐related reactions. “We prefer the liposomal form since it is safer, more effective, and has lesser side effects. The flip side being that it is more expensive,” Dr. Akshay Nair, an eye surgeon from Mumbai, told BBC News.
This has led to families having to spend upwards of Rs. 3 lakhs for one individual’s treatment — assuming the lowest possible number of vials are prescribed to them for the shortest possible duration.
According to the U.S. Centers for Disease Control (CDC), mucormycosis is a rare but serious mold infection that is caused by a group of molds called mucormycetes. The infection can cause vision loss, damage to the nose and jawbones, and — in the most severe cases, where the fungus makes its way to the brain — death. While diabetic and immunocompromised Covid19 patients are especially vulnerable to mucormycosis, the use of steroids for treatment is believed to be heightening the risk of the infection. Although the disease is treatable if detected early, the shortage of drugs to facilitate that is making the prospect grim.
At present, the rate of mucormycosis infections in the Indian population isn’t high per se — with 140 cases per million people — but hospitals are starting to report a 10 to 15-times rise in the number of cases. Moreover, its mortality rate among those infected is an alarming 38%. “The frequency with which we are witnessing the occurrence of Covid19-triggered mucormycosis with high morbidity and mortality is alarming,” Dr. Manish Munjal, a senior E.N.T. surgeon at Sir Ganga Ram Hospital in Delhi, told The Indian Express when the first cases of mucormycosis in Covid19-patients were reported in December last year.
In the meantime, Rajasthan declared the outbreak of black fungus an “epidemic” yesterday with the Sawai Man Singh (SMS) Hospital in Jaipur, the state capital, housing around 100 patients in a separate ward at present. The decision was prompted by the need to ensure integrated and coordinated treatment of mucormycosis in Rajasthan, the state’s health minister, Raghu Sharma, said. Delhi, Haryana, and Karnataka are among other states trying to tackle the outbreak by setting up expert committees to explore better prevention and treatment options.
In addition, due to fact that mucormycosis can lead to significant permanent damages like loss of vision and hearing, besides disfigurement, medical professionals are advising Covid19 patients experiencing one-sided headaches, facial pain, and difficulty chewing or swallowing, to seek help immediately. “Early clinical suspicion on symptoms such as nose obstruction, swelling in the eye or cheeks, and black dry crusts in the nose should immediately prompt a biopsy and start of the anti-fungal therapy as early as possible,” Dr. Munjal said.
Devrupa Rakshit is an Associate Editor at The Swaddle. She is a lawyer by education, a poet by accident, a painter by shaukh, and autistic by birth. You can find her on Instagram @devruparakshit.
Related

Bubonic Plague Increased Immunity in Future Generations, Research Suggests