
Everything You Need to Know About Gonorrhea
From symptoms, to how likely you are to get it.
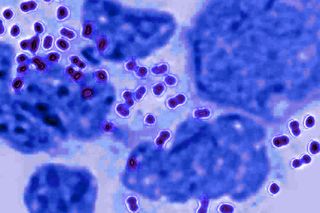
Gonorrhea is a common sexually transmitted infection (STI) that may or may not develop noticeable symptoms. Women, especially, are not prone to obvious symptoms. The disease — often colloquially referred to as ‘The Clap’ — used to be easily treatable by antibiotics, but the number of antibiotics that can be used to treat it are fast dwindling, as resistant strains are on the rise in India and around the world.
What is gonorrhea and how is it transmitted?
Gonorrhea is a disease caused by a bacteria called Neisseria gonorrhea. It is transmitted via vaginal, anal or oral sex. It is also transmitted from skin-to-skin contact with infected genitals, even if there is no penetration, orgasm or ejaculation. It is not communicated by casual personal contact, however, or by contact with any object touched or used by an infected person, as the bacteria cannot live for long outside the human body.
It can be passed by a pregnant woman to her baby during a vaginal birth (not a C-section) and most commonly affects the eyes of babies infected with the bacteria. Gonorrhea can cause blindness and other serious health problems for newborns, so testing for and treating an infection during pregnancy is preferable.
How prevalent is gonorrhea? Is there a way to avoid it?
According to the World Health Organization (WHO), 500 million new cases of one of four curable STIs (chlamydia, gonorrhea, syphilis and trichomoniasis) occur each year worldwide. In India, estimates place the prevalence of gonorrhea at 6% of the population (that’s 1 in every 17 people), though it may be more common, as many cases of gonorrhea go undiagnosed. Gonorrhea, like most STIs, tends to be more prevalent in urban areas, and among young adults, who are more likely to be sexually active with multiple partners without using protection — all risk factors for STIs.
That said, anyone who has sex with someone with a gonorrhea infection can catch gonorrhea. Using condoms or dental dams (a piece of thin, soft plastic or latex) are the best preventative methods, though they are not guarantees against the infection.
What are the symptoms of gonorrhea?
Gonorrhea can infect the cervix, anus, penis, throat or eye, depending on what part of the body was exposed to the bacteria. Infections often don’t develop noticeable symptoms; this is especially true for women. When an infection does manifest symptoms, signs of gonorrhea vary between men and women.
In men, gonorrhea symptoms may include:
- white, yellow or green pus-like discharge from the penis tip
- pain or burning during urination
- a painful or swollen testicle(s)
In women, gonorrhea symptoms may include:
- more vaginal discharge than usual
- bleeding outside the menstrual cycle
- pain or burning during urination
- pelvic or abdominal pain
- pain during sex
In both men and women, depending on the location of infection, gonorrhea symptoms may include:
- a sore throat and swollen lymph nodes
- an itchy anus, a sore anus, pus-like discharge from the rectum, and straining, pain and/or blood spotting during bowel movements
- eye sensitivity to light, eye pain, and pus-like discharge from the eye(s)
An untreated gonorrhea infection can spread to your joints, a complication known as gonococcal arthritis; symptoms of this gonorrhea complication include: warm, stiff, swollen and painful joints, especially during movement. Similarly, the infection can also spread to the blood and other body parts and cause rashes or skin sores.
An untreated gonorrhea infection can cause fertility problems for both men and women. In men, epididymitis, that is, an inflammation of a portion of the sperm ducts inside the testicles, might be a symptom of an untreated gonorrhea infection. In women, an untreated gonorrhea infection can spread to the the upper reproductive tract and develop into pelvic inflammatory disease (PID). Both of these painful conditions can damage fertility.
How do you get diagnosed?
Gonorrhea is typically diagnosed by a simple urine test, though in some cases health care providers may recommend a swab of the infected area.
As with most STIs, if you’ve been diagnosed with a gonorrhea infection, it’s important that your current sexual partner and any other recent sexual partners be informed, tested and treated to help stop the spread of the infection. And it’s advisable to get tested for gonorrhea, and all other STIs, after any unprotected intercourse with a new sexual partner.
What is the treatment for gonorrhea?
Gonorrhea is typically treated by an antibiotic injection accompanied by one of two possible oral antibiotics. However, many strains of the bacteria are multi-drug resistant, and there are few antibiotics left that will reliably treat an infection. In March of this year, a UK man was diagnosed with the “worst-ever” case of “super-gonorrhea” that wasn’t treatable with common antibiotics, thought to have been contracted in Southeast Asia. (There is some evidence that suggests gonorrhea infection in men is more likely to be resistant to antibiotics.) That said, there are promising new treatments on the horizon, but they are still far from any kind of regulatory approval or public access.
If you have taken your full course of treatment and still show symptoms, consult your doctor again.
Doctors usually recommend not having sex during treatment and for at least seven days after treatment concludes and until your current sexual partner has finished their treatment.
Can gonorrhea be cured?
Right now, yes; even the “worst-ever” case finally responded to a niche antibiotic. But treatment does not offer immunity for the rest of your life; it is entirely possible to contract gonorrhea more than once, especially if you’re not using condoms or dental damns with new sexual partners.
This is part of The Swaddle’s series on sexually transmitted infections.
Liesl Goecker is The Swaddle's managing editor.
Related


The Postpartum Complication Often Mistaken for New‑Mom Stress, or Postpartum Depression
