
Everything You Need to Know About Ectopic Pregnancies
Without treatment, an ectopic pregnancy can rupture the Fallopian tube and cause life-threatening internal bleeding.
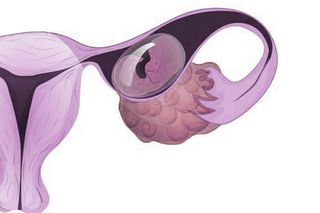
We all know the science behind a normal pregnancy: the fertilized egg moves from the Fallopian tube to implant itself into the uterus — the uterine lining, to be more precise. If this happens, the process of conception is considered to have been successful.
But, in the case of an ectopic pregnancy, the embryo instead ends up somewhere else, such as in the Fallopian tube, the abdominal cavity, or the cervix.
If left untreated, an ectopic pregnancy, say, in the Fallopian tube, could rupture the tube, which is not designed to accommodate a growing fetus. It could also lead to severe, life-threatening internal bleeding.
Dr. Shashikala Hande, a consultant obstetrician and gynecologist at Bengaluru’s Cloudnine Group of Hospitals, notes that mortality rates from ectopic pregnancies have declined by 80%, likely due to early detection and intervention, in an op-ed recently written for the Indian Express.
However, an early diagnosis is not always possible because “an ectopic pregnancy takes place within the first few weeks of the pregnancy, mostly unknown to the mother,” says Dr. Hande.
Related on The Swaddle:
How to Get Pregnant (Besides the Obvious)
What are the signs and symptoms of an ectopic pregnancy?
Some of the signs, Dr. Hande says, could include vomiting, weakness, shoulder, neck or pelvic pain. While these are common with a normal pregnancy, some signs that might prompt you to consult a doctor include looking for vaginal spotting of blood, extreme abdominal cramps, or pain on one side of the abdomen or in the rectum.
Why do ectopic pregnancies occur?
It’s difficult to know the exact cause of an ectopic pregnancy because there are many potential causes that aren’t always clear from the beginning. They include inflammation and scarring of the Fallopian tubes from a previous infection, surgery, or hormonal factors. It could also be due to genetic abnormalities, birth defects in the mother that affect the shape and condition of the Fallopian tubes and reproductive organs.
How is an ectopic pregnancy diagnosed?
Ectopic pregnancies can’t be diagnosed through a physical exam. They are usually diagnosed through a transvaginal ultrasound, to assess whether the gestational sac is intact, and a blood test. If levels of hCG and progesterone — the two hormones that are present during pregnancy — are found to be fluctuating, for instance, decreasing or even remaining steady for a few days into the pregnancy, then chances are that the pregnancy is ectopic.
In extreme cases, when one of the symptoms is significant pain or bleeding, a doctor may not have enough time to do either of the above because the chance of a Fallopian tube rupturing is high. In that case, a doctor may need to perform an emergency surgery.
Related on The Swaddle:
Bleeding During Pregnancy: What’s Normal, What’s Not
How are ectopic pregnancies treated?
Usually, ectopic pregnancies are treated in one of two ways: 1) medication that causes symptoms similar to that of miscarriage, such as cramping, bleeding and the passing of tissue, or 2) a surgery to remove the embryo and repair any internal damage.
Is there a way to avoid an ectopic pregnancy?
It isn’t possible to predict or prevent every case of an ectopic pregnancy, but maintaining good reproductive health may help in reducing its chances. This includes using condoms to reduce the chances of contracting sexually transmitted infections, getting regular gynecological exams and screening for STIs.
What implications does an ectopic pregnancy have on future pregnancies?
Dr. Hande says that the chances of a recurring ectopic pregnancy are 10%. “Surgery may scar the fallopian tubes, and it can make future ectopic pregnancies more likely. If the removal of one or both Fallopian tubes is necessary, speak to your doctor about possible fertility treatments. Remember that many women go on to have healthy pregnancies and babies. When you’re ready, talk to your doctor about ways you can ensure that your future pregnancy is a healthy one,” recommends Dr. Hande.
Anubhuti Matta is an associate editor with The Swaddle. When not at work, she's busy pursuing kathak, reading books on and by women in the Middle East or making dresses out of Indian prints.
Related


Extreme Period Pain, or Acute Dysmenorrhea, Is a Real Health Issue
